See all > Preventative health and wellness
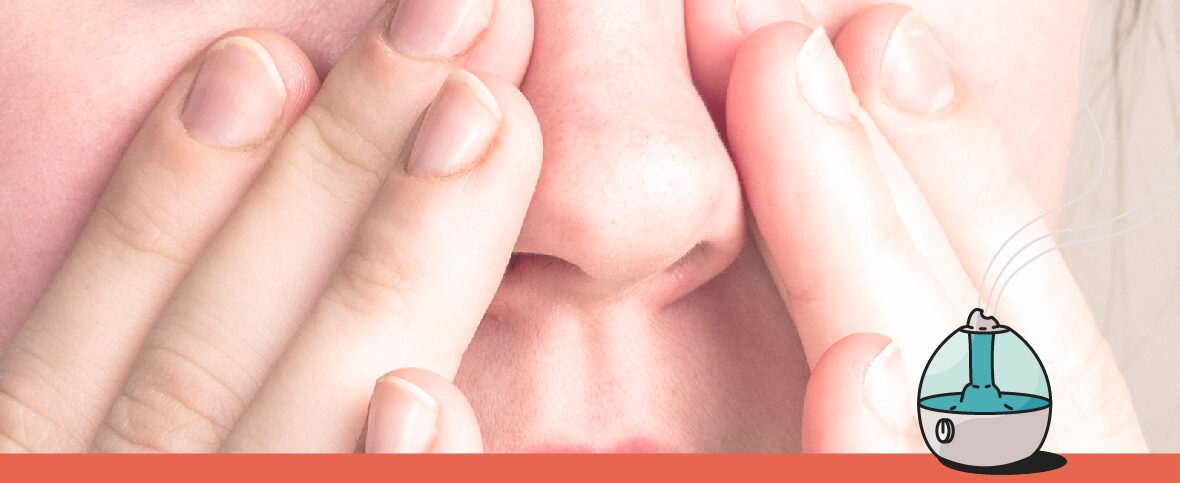
Why do I get a sinus infection (sinusitis) every fall?
Having a sinus infection is basically a guaranteed way to spend a lot of time feeling lousy. Its throbbing ache can make it hard just to get through the day. But there are ways of easing your discomfort. Here’s how to treat your sinus infection at home and how to know when it’s time to call in the professionals.
What’s a sinus infection?
Your sinuses are four connected, hollow cavities inside your face. You’ll find them just behind your nose — two right above your eyebrows and two below your eyes.
Normally, your sinuses are filled with air. Since their job is to produce the mucus that lines the inside of your nose, they’re bordered by tiny hairs called cilia that are constantly sweeping mucus through the area and down your throat.
Sometimes, however, the linings of your sinuses become inflamed. This makes it difficult for the mucus to drain properly, and can cause it to back up. This, in turn, creates the perfect environment for germs to grow, leading to — you guessed it — a sinus infection.
What are the signs of a sinus infection?
While some symptoms of sinusitis overlap with those of a cold, sinus infections result in more pain and discomfort in the central part of your face. Signs of a sinus infection include:
- Pain, tenderness, pressure, or all three in the area around your eyes, forehead, cheeks, and nose
- Lots of nasal discharge, especially if it’s thick and yellow or green
- Fluid drainage in the back of your throat — this can trigger you to swallow or cough excessively
- Difficulty smelling or tasting, or loss of sense of taste or smell
Less often, you may also experience:
- Bad breath
- Fever
- Cough (especially when lying down)
- Tooth or gum pain
- Ear pressure or pain
- Feeling tired
- Headache
Any of the following symptoms are a red flag that you need urgent care:
- Pain or swelling around your eye
- High fever
- Altered mental state with fever
- Painful eye movements
- Vision changes or vision loss
How weather changes can affect your sinus health
You’re probably not a fan of being snotty, but the goo your nose produces is there to keep you healthy. Mucus lubricates the inside of your nasal passages and helps warm and humidify the air you breathe.
It’s also a major line of defence between you and any pathogens in your environment. Mucus acts as your lung’s filter, keeping out foreign substances like bacteria, dirt, and viruses.
Weather changes can disrupt these important processes, however. The cold, dry outdoor air and dry indoor heating rob your mucus of its moisture, transforming it into dried-up, clumpy mucus that’s more liable to block your nasal passages and obstruct your breathing. It can also cause irritation, and even make your nose bleed.
Furthermore, cold weather slows down your sinus cilia, so they function less effectively. This causes some of the mucus to roll forward out of your nose instead of down the back of your throat. So, if you find that your nose starts to run the minute the temperature drops, you’re not imagining it.
Temperature isn’t the only external force affecting your sinus health. Changes to bariatric pressure, like before a thunderstorm, can also upset them. Some people find these air pressure changes so significant that they cause sinus headaches.
Can fall allergies cause constant sinus infections?
If you feel like you’ve had a sinus infection since ragweed season started, there’s a reason.
When you have seasonal allergies, your body’s immune system produces inflammation in response to otherwise harmless substances — like pollen. This immune response causes swelling inside your nasal cavity, making it harder for mucus to drain as it normally does. It also prompts your body to increase its production of mucus.
Since seasonal allergies persist for quite a while, your body deals with inflammation and elevated mucus levels for long periods. This increases the likelihood that you’ll develop a sinus infection. And, if you already have one, the ongoing inflammation and jump in mucus production make it more difficult to resolve.
Even worse, the antihistamines you take to counteract your allergies can actually be part of the problem. These medications dry up mucus to stop your nose from running as much. But, an unfortunate by-product of this can be a thickening of your mucus, preventing it from draining as easily.
Fall allergies or sinus infection?
Telling the difference between fall allergies and sinus infections can be challenging. Not only does one often result in the other, they also share a central symptom — the stuffy nose. There are, however, some important differences.
Fall allergies often include itchy, watery eyes and sneezing. They might also leave you wheezing or coughing.
Sinus infections also distinguish themselves from allergies through the pressure, pain, or discomfort that you feel in the middle part of your face. Additionally, they result in thick and sometimes even neon-coloured snot.
And, if you’re experiencing bad breath or fever, you’re likely dealing with sinusitis. While these symptoms occur less often with a sinus infection, they definitely don’t happen with allergies.
Are sinus headaches common in the fall too?
If you experience fall allergies, the answer to this is yes. The more your allergies act up, the more inflammation you’ll experience, and the more fluid is likely to build up in your sinuses.
Since the pressure from the fluid buildup triggers the sinus headache, these are more likely to flare up when your fall allergies do. However, what seems like a sinus headache might not always be one.
Sudden changes in barometric pressure, which you see more of in the fall, can cause sinus pain, and even trigger migraines in certain individuals. Since you’re more likely to experience these shifts during seasonal transitions, you might see a spike in migraines too. To make it even more confusing, allergies can be a migraine trigger for certain individuals.
The bottom line is that it can be hard to tell the difference between a migraine and a sinus headache. Both cause facial pain and tenderness, and both get worse with allergy exposure. Ultimately though, since the two conditions require distinct treatment methods, your best bet is to speak to a doctor if you’re not sure which one you’re grappling with.
What’s the best medication for a sinus infection?
Treating a sinus infection depends on its underlying cause. If your sinus infection hasn’t improved around day seven, it may be the result of a bacterial infection. In these cases, your doctor will likely write you a prescription for an antibiotic like amoxicillin (Novamoxin or Polymox).
Or, if you have a penicillin allergy, they might choose levofloxacin (Levaquin). Azithromycin (Zithromax) was a go-to, but it isn’t recommended these days due to high rates of resistant bacteria.
However, most sinus infections aren’t bacterial, so antibiotics won’t work. Often, sinusitis is the result of a virus, nasal polyps causing a blockage, or allergies triggering inflammation. In these cases, treatment should instead center on addressing symptoms and treating the underlying cause.
To help with any soreness and discomfort, take an over-the-counter (OTC) pain reliever like ibuprofen (Advil) or acetaminophen (Tylenol). And, you can use a saline rinse or neti pot to help you flush out all that snot and relieve some of the discomfort. Just make sure to use sterile or bottled water instead of tap to avoid other problems like amebic encephalitis — that’s right, brain-eating amoebas.
For temporary relief of congestion, you can opt for blowing your nose in a steamy shower. Steaming your face with a clean mould-free source, regularly applying a wet and warm cloth to it, and sleeping with a couple of pillows underneath you to elevate your head is also helpful.
Finally, make sure you’re staying hydrated. Getting in enough fluids will keep your nasal mucus from becoming too thick and gloopy. And, as with any illness, getting plenty of rest helps your body heal.
If you’re trying all of this and you’re not getting better after 10 days, it’s a good idea to seek medical treatment. While most acute cases of sinusitis resolve on their own, in severe or chronic cases you may require prescription steroids. These are available in intranasal spray or oral tablets, and work by counteracting inflammation, reducing your pain and making it easier for mucus to drain.
How can I prevent a sinus infection in the fall?
Most sinus infections are the result of allergies or a virus. So, the best way to prevent them is to avoid getting sick or having allergies in the first place.
If you’re able to properly manage your allergies on your own, great! Make sure to start taking your allergy medication before your fall allergies hit to head off symptoms before they start. If you’ve traditionally had more trouble dealing with what fall has in store for you, however, it’s probably time to see an allergist.
An allergist can advise you on the best treatment for your allergies, whether that’s a specific medication, lifestyle adjustments, or immunotherapy.
When it comes to your immediate environment, using a humidifier is a really simple but effective way to keep dry air at bay inside. Whether you have a sinus infection or not, this will help to ease any nasal discomfort.
And finally, while you can’t keep yourself from getting sick completely, incorporating good hand hygiene is a great start. Beyond that, protect yourself from the flu by getting vaccinated and maintaining a healthy immune system.
When to see a doctor for your sinus infection
Most cases of sinusitis clear up within a week or two. While you might feel some discomfort, managing your sinus infection with OTC pain medications, steam, and other home treatments should work.
If you’re dealing with chronic sinusitis, however, or if your infection is making it hard to breathe, it’s time to see a doctor. In severe cases, a doctor can prescribe steroids to ease your swelling, helping to relieve your symptoms.
Even if you’re not dealing with breathing issues, if your infection isn’t getting better after 10 days, it’s time to speak to a healthcare provider. They can help determine if you have a bacterial infection that needs treatment with antibiotics.
If you’re dealing with a stubborn sinus infection Maple can help. Maple is a telehealth platform that connects you with Canadian-licensed doctors and specialists from your phone, tablet, or computer. With Maple, you can connect to an online doctor for advice on your treatment options, and to help you address the underlying causes of your sinusitis.
Don’t muscle through the discomfort of a sinus infection alone. Reach out to speak to a doctor today and help take the pressure off your sinuses.
The information presented here is for educational purposes and is not meant to replace the advice from your medical professional.
When using virtual care, all medical treatment is at the sole discretion of the provider. Virtual care is not meant for medical emergencies, and your provider will determine if your case is appropriate for virtual care. If you are experiencing an emergency like chest pain or difficulties breathing, for example, please call 911 or go to your nearest emergency room.
Trusted by millions of Canadians
Get started now
We're trusted by millions of Canadians
Join millions of Canadian families who enjoy 24/7 access to medical care within minutes.
Get started now4.6 score
5K+ Trustpilot reviews
Do you need medical care today?
Trusted, experienced doctors and nurse practitioners are ready to see you.
