See all > Parenthood
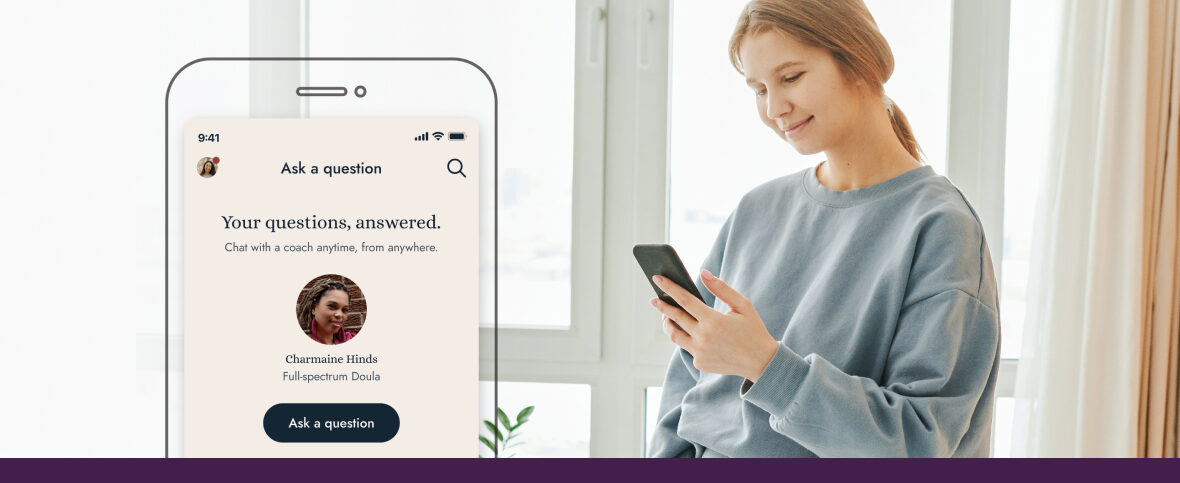
Navigating challenging and high-risk pregnancies
Finding out you’re pregnant can be a joyful and exciting event. For many people, however, pregnancy comes with hardships. Many experience fertility challenges – one in four pregnancies end in miscarriage – or have issues accessing healthcare providers. On average, Canadians wait five months to see a family health specialist.
Over 350,000 people in Canada gave birth last year — and it wasn’t always an easy path to get there. While many birthing parents experience pregnancies and deliveries free from complications, others encounter complex obstacles.
Analyzing data from more than 3.1 million pregnancies across Canada, a study by The Hospital for Sick Children (SickKids), Sunnybrook Health Sciences Centre, and the Institute of Health Policy, Management and Evaluation at the University of Toronto (IHPME) found that mothers under the age of 19 or over 30 were at increased risk for severe maternal morbidity and mortality. The highest risk was for women over the age of 44, a very advanced maternal age, while mothers aged 20 to 24 had the lowest.
With birth demographics changing, the age of mothers giving birth has increased, leading to more pregnancies in those of advanced maternal age (over the age of 35).
The resulting changes in pregnancy care and outcomes is forcing parents and businesses to evolve and adjust to today’s definition of parenthood. Simply put, supporting mainly young heterosexual couples with no mental or physical health issues doesn’t actually help today’s new parents.
What’s a high-risk pregnancy?
A high-risk pregnancy involves increased health risks for either the birthing person, the baby, or both. Pregnancies can begin as a high-risk pregnancy – when the birthing person has pre-existing medical conditions – or evolve gradually or suddenly into a high-risk pregnancy involving fetal, placental, or other complications.
Factors that may make a pregnancy high-risk include:
- Pre-existing health problems like depression, diabetes, cancer, high blood pressure, kidney disease, or epilepsy
- Use of alcohol, tobacco, or illegal drugs
- Intimate partner or domestic violence
- Maternal age younger than 17 or older than 35
- Multiple pregnancies (e.g. carrying twins or triplets)
- History of three or more miscarriages
- Carrying a baby with a genetic condition such as Down syndrome or a heart, lung, or kidney problem
- History of previous pregnancy complications, such as preterm labour or birth, pre-eclampsia or seizures (eclampsia), or having a baby with a genetic disorder
- An infection such as HIV, Hepatitis, cytomegalovirus (CMV), chickenpox, rubella, toxoplasmosis, syphilis, or COVID-19
The reality is that growing a family — and doing so amidst a global pandemic over the last two years — is not easy for many.
A study polling 2,000 U.S. families found that 58% of new parents are overwhelmed by the sea of impersonal options when it comes to family health. Moreover, 80% of new or expecting parents rely on online search or other forms of non-evidence-based resources for information that often leads them astray.
What you should do if your pregnancy is high-risk or particularly challenging
If you or your partner are currently experiencing a higher-risk pregnancy, here are some useful tips to consider:
- You may need additional medical care for the birth available in a hospital, as opposed to a birthing centre or at home. For rural parents, this may require travel.
- Your care provider may also recommend additional imaging and tests, including, but not limited to, ultrasounds, genetic screening, blood tests, and a consultation with an obstetrician.
- Make sure you’re taking a high-quality prenatal vitamin that provides at least 16 to 20 mg of iron and 0.4 mg of folic acid, calcium, and vitamin B12.
- Beyond your primary care provider, whether it’s a family doctor, OBGYN, or midwife, consider other people who could join your support team, including a doula or family members. A doula is an emotional support person who can help guide you through pregnancy, postpartum, or both.
- Keep in mind that one in five women will experience a mood disorder either during pregnancy or postpartum. The Cognitive Behavioural Therapy framework is one tool you can use to fight anxious thoughts. Ask yourself:
1. What is the kernel of truth in my anxious thoughts?
2. What evidence do I have to support or disprove this thought?
3. What’s an alternative way for me to think about this?
4. What would I tell a friend if they told me they were feeling the same way? - Consider adding a pelvic floor physiotherapist (PT) to your care team. Preventatively working with a physiotherapist during pregnancy can help manage urinary incontinence, strengthen the pelvic floor, and prevent or treat pelvic organ prolapse and diastasis recti.
- If you have nutritional concerns, consider working with a registered dietitian or naturopathic doctor. Research shows that parents who introduce preventative measures in their pregnancy show fewer postpartum thyroid complications. A high-quality prenatal vitamin, which can also be taken after birth, may already include many micronutrients required to maintain your thyroid health.
- Know that one in four pregnancies end early in miscarriage. Factors that impact the risk of miscarriage are genetic abnormalities (which are out of a parent’s control), advanced maternal age (due to changes in egg quality over time), undiagnosed medical conditions like hypothyroidism, high blood pressure, or celiac disease, binge drinking, and infections.
Lastly, if you experience any of the following symptoms during pregnancy, speak to a medical professional immediately:
- Vaginal bleeding
- Noting a decrease in your baby’s movements
- Severe abdominal pain or cramping
- Symptoms of prenatal anxiety or depression, such as thoughts of self-harm or harm to your baby
- Severe headaches
- Fever and/or chills
How your workplace can support new parents
Workplaces have an important role to play as an employee goes through the various stages of pregnancy and parenting — everything from implementing inclusive work policies to creating safe spaces amongst managers and staff.
Here are some things your workplace can do to support employees who are growing their families:
- Make sure language surrounding parental benefits, as well as the benefits themselves, are inclusive of all types of families — whether they’re being formed through pregnancy, adoption, or surrogacy
- Plan a parental benefits strategy that covers all stages: conception and/or adoption navigation, fertility support and/or treatment, bereavement leave, termination support, prenatal education, care provider navigation, guidance on employment insurance or income top-ups, clear information on your company’s leave policies, postpartum education and/or support, and early childhood programs
- Remember that parental benefits programs should support parents (the birthing parent and co-parent) as well as the new baby — many programs mistakenly design solely for the latter
- Coach managers on how to support employees who disclose their family plans and/or intentions of pregnancy and parental leave
- Coach managers to have open conversations on how, if at all, the employee would like to be kept informed of business changes while on leave
- Build or provide a private and comforting space for pumping or nursing
There’s a lot to know about navigating challenging and high-risk pregnancies, but with the right kind of support, many families go on to have healthy deliveries and babies.
If you have a high-risk pregnancy, it’s crucial to reach out for support from a healthcare provider so that you and your baby can get the care you need.
The information presented here is for educational purposes and is not meant to replace the advice from your medical professional.
When using virtual care, all medical treatment is at the sole discretion of the provider. Virtual care is not meant for medical emergencies, and your provider will determine if your case is appropriate for virtual care. If you are experiencing an emergency like chest pain or difficulties breathing, for example, please call 911 or go to your nearest emergency room.
* The term “birthing parent” was used in this article to refer to anyone who physically delivers a baby. We acknowledge this isn’t the only path to parenthood.
This blog was co-written by Maple and Koble, a health app for new and expecting parents. If you’re a Maple user, you can get preferential pricing for Koble.
Trusted by millions of Canadians
Get started now
We're trusted by millions of Canadians
Join millions of Canadian families who enjoy 24/7 access to medical care within minutes.
Get started now4.6 score
5K+ Trustpilot reviews
Do you need medical care today?
Trusted, experienced doctors and nurse practitioners are ready to see you.
