Polycystic ovary syndrome (PCOS) is a hormonal disorder that affects up to 10% of women and up to 25% of trans men of reproductive age. Despite how common PCOS is, it’s widely misunderstood. That might be because PCOS presents differently across patients. There’s a constellation of possible symptoms you can experience, making this syndrome hard to predict and diagnose.
PCOS patients can be treated by endocrinologists — doctors who specialize in hormone disorders — as well as family doctors or gynecologists. The glands in your body that secrete hormones make up your endocrine system. And what are hormones? They're chemical messengers that communicate between your organs and tissues. They’re vital for bodily functions like digestion, metabolism, and reproduction. When your hormones are out of imbalance there be ripple effects all throughout your body.
What is polycystic ovary syndrome?
PCOS is a hormone imbalance where people with female reproductive systems have higher than normal levels of androgens, a group of hormones that fuel male characteristics. In teenage boys, androgens drive changes like facial hair growth, deeper voice tenor, and broadening of shoulders.
Based on the name "polycystic ovary syndrome", you’d be justified in thinking that the hormone imbalance stems from cysts on your ovaries. But, you don’t need to have ovarian cysts to have PCOS. If you match other signs, like biochemical or clinical criteria we explain further below, the diagnosis may be confirmed whether you have cysts or not.
Why do women have male hormones? Healthy ovaries naturally produce a small amount of androgens, as do your adrenal glands. With PCOS, your ovaries and adrenal glands produce higher levels of androgens. The increase in androgens can cause physical symptoms like increased body hair growth, menstrual irregularity, and acne. PCOS and it’s complications can also lead to future health problems like diabetes and heart disease.
What causes PCOS?
PCOS has been called “a collision between blood glucose regulation and reproductive hormones.” For people who are insulin resistant, their bodies have a hard time using glucose efficiently. As a result, glucose builds up in their bloodstream and creates high blood sugar levels. High blood sugar levels increase the amount of androgens your body produces. The outcome? Hormonal imbalance, the hallmark of PCOS.
Being overweight is a risk factor for insulin resistance. But, even lean people who have PCOS usually test positive for insulin resistant.
If a patient is overweight, weight loss for PCOS may improve symptoms. Doctors recommend that patients think of weight loss from a lifestyle-based approach. Eating lots of whole plant foods, complex carbohydrates, and unsaturated fats is a good diet to improve insulin resistance. Low to moderate intensity exercise can also help you feel your best. Since PCOS is a lifelong condition, a healthy lifestyle will help manage symptoms long term.
While there are well-documented contributors to PCOS, it’s important to note that researchers haven’t found a clear-cut cause. Genetics, lifestyle factors, inflammation, and insulin resistance are all associated. But, there’s no way to tell for sure whether or not someone will develop PCOS. It’s all down to your individual endocrine system.
PCOS signs and symptoms
There are several signs and symptoms that are often seen with PCOS. They include:
- Irregular periods
- Lack of periods
- Increased hair growth (hirsutism), typically on the face, chest, back, or buttocks
- Thinning scalp hair
- Oily skin or acne
- Weight gain, especially around the waist
- Depression, anxiety, and mood swings
- Darkening of skin around the neck, groin, underarms, or skin folds (acanthosis nigricans)
- Increased blood sugar
- Difficulty conceiving/infertility
What is the difference between an ovary with PCOS and a normal ovary?
As mentioned above, you don't have to have ovarian cysts to qualify for PCOS. The reverse is also true. Having cysts on your ovaries doesn’t automatically signify PCOS.
Let’s say you’re looking at an ultrasound of a PCOS patient, and there are cysts present. One or both ovaries will contain small, immature ovarian follicles. These follicles will show up in medical imaging as cysts.
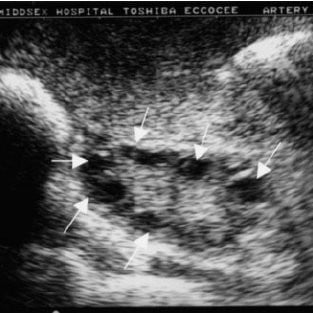
With PCOS, ovarian follicles stay in an immature state because of abnormal hormone levels present in the person’s body. These follicles can't grow to their fully matured state where an egg would normally be released. Instead, the immature follicles accumulate in the person’s ovaries.
Some people have 12 or more cysts present in their ovaries. The good news is that the number of cysts you have tends to decrease with age. And, symptoms can often be improved through medical help and lifestyle adjustments.
PCOS diagnosis and treatment
Diagnosing PCOS is an inexact science. In fact, it’s a diagnosis of exclusion, meaning that doctors need to rule out all other possible causes for your symptoms before providing a PCOS diagnosis. There are no definitive tests that doctors can perform to absolutely confirm or deny that their patient has the syndrome.
Doctors diagnose PCOS based on the Rotterdam criteria. If a patient has two out of three criteria present, a diagnosis of PCOS can be given.
The Rotterdam criteria are:
- Irregular periods.
- Increased androgen levels.
- Cysts found on ovaries, confirmed by ultrasound.
Some tests doctors rely on are:
- Pelvic exams — a doctor visually or manually inspects their patient’s reproductive area to check for noticeable cysts, growths, or other abnormalities.
- Blood tests — tests check for hormone levels, insulin resistance, and other markers like fasting cholesterol levels.
- Ultrasound — a form of medical imaging that allows doctors to inspect the ovaries and uterine lining of their patient.
Since PCOS is different for every patient, treatment for polycystic ovary syndrome also has to be individually targeted. Doctors will recommend different options to relieve their patient’s symptoms and concerns. These options include:
Medication
While there aren’t specific PCOS medications, doctors will often prescribe what’s most useful for treating your unique concerns. The combination birth control pill can help regulate your periods. If you’re looking to remain fertile, your doctor might prescribe ovulation medications to help balance your hormones. Diabetes medications like metformin can help with insulin resistance. And for hirsutism, a blood pressure medication called spironolactone can be prescribed.
Lifestyle changes
Since PCOS is linked to obesity and insulin resistance, improving these health markers can greatly reduce symptoms.
How to get pregnant with PCOS
PCOS is one of the most common causes of infertility since it disrupts normal reproductive system functioning. But, the vast majority of people with PCOS can get pregnant with proper treatment.
A combination of fertility treatments and lifestyle adjustments will allow most people with PCOS to conceive. In rare cases, a patient may require more intensive fertility treatments.
Can PCOS go away after pregnancy?
PCOS won’t automatically go away after pregnancy if the underlying issues are still present. Plus, the arrival of a baby and the onset of breastfeeding can further alter a mother’s hormone balance and add new stress to her life.
PCOS is a lifelong condition. It usually emerges around the time someone has their first period. If you’re diagnosed with PCOS, you’ll always need to manage the condition.
How to get help for PCOS
Even though PCOS is a common endocrine disorder, it’s shrouded in mystery and misconceptions. Like with other chronic illnesses, its invisibility can make people with the condition feel alone. People with PCOS often feel like they have to handle the weight of regular life, plus their difficult symptoms at all times.
It’s important to get medical help for PCOS if you suspect you have it. PCOS can lead to outcomes like diabetes and heart disease in the long run as well as endometriosis and an increased risk of endometrial cancer. Plus, people who want to conceive will find it much easier to do so if they take steps to address their condition beforehand.
To get help for PCOS, talk to your doctor about your concerns. List the symptoms you’ve been having, your medical history, and any medications you’re currently or have recently been on. Keep a record of your menstrual cycle as well.
Your doctor may recommend some of the tests mentioned earlier in this article. They may also refer you to an endocrinologist, who can give a more expert assessment of your hormone health. Referrals for a PCOS endocrinologist may result in being put on a lengthy wait list. If you’d prefer to fast-track your appointment with an endocrinologist, our doctors are ready to help.
The information presented here is for educational purposes and is not meant to replace the advice from your medical professional.
When using virtual care, all medical treatment is at the sole discretion of the provider. Virtual care is not meant for medical emergencies, and your provider will determine if your case is appropriate for virtual care. If you are experiencing an emergency like chest pain or difficulties breathing, for example, please call 911 or go to your nearest emergency room.
